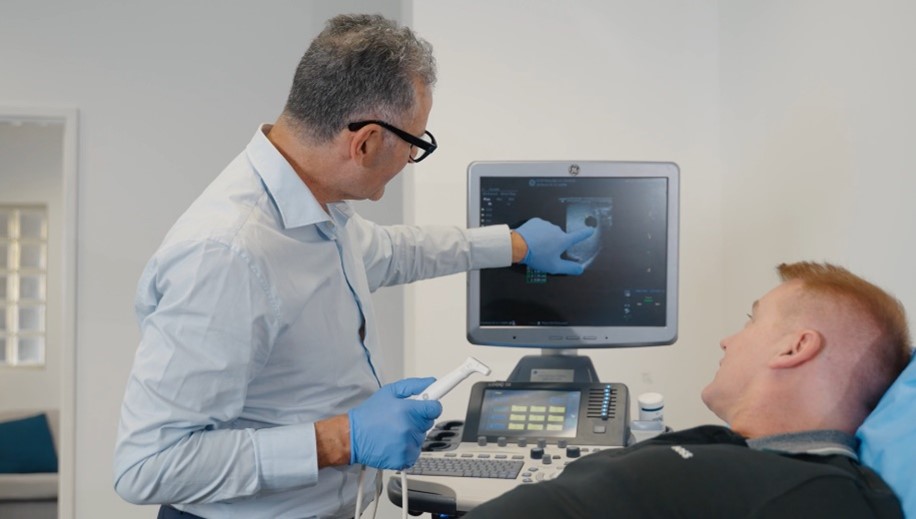
Open-ended, No Scalpel and traditional vasectomies
Open-ended Vasectomy
A true open-ended vasectomy should take at least 25 minutes to perform.
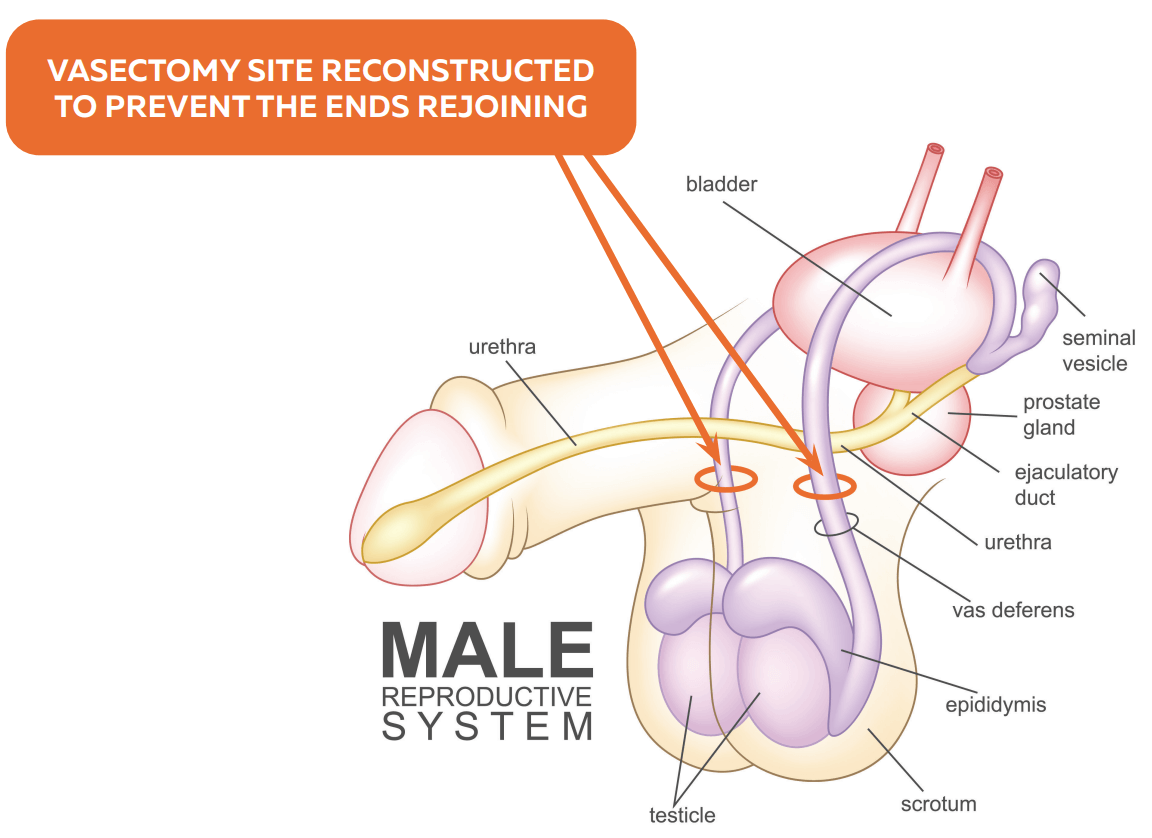
This procedure involves two tiny incisions to access the vas tubes. The tubes are then cut, and the testicular end is left opened and unsealed, with both ends of the tubes separated by layers of tissue within the scrotal sac by fine suturing. Sperm continues to be produced after the vasectomy so this fluid travels from the testicle up the vas where it then flows out of the vas and into the tissues. The body reabsorbs this naturally. The testicular vas deferens and the vas deferens that leads to the prostate reconstructed in separate compartment to minimise the risk of failure.
As a result of this technique:
- Sperm does not suddenly build up in the testicle, so the development of an inflammatory cascade, blow out and scarring of the fine epididymal tubules is avoided.
- Sperm flow is directed and absorbed under the skin rather than left to clog up the tubules.
- An open-ended vasectomised patient is unlikely to be aware that they have had a vasectomy unlike the closed ended vasectomy patients that often experience some form of aching and tenderness.
- The nature of this technique prevents the build-up of sperm and the associated congestion (post vasectomy pain syndrome), a lower rate of postoperative pain, and a better potential for vasectomy reversal in the future.
- It is important to use contraception for the first few months after surgery. This is done to allow the remaining sperm to be flushed out beyond the scrotal ties. It is important to note that sperm will continue to be produced in the testicles after surgery.


No Scalpel Vasectomy
A “no scalpel” technique merely describes how the vas tubes are accessed. Once the skin is opened, a traditional technique is generally used to perform the vasectomy.
A “no scalpel” technique involves tearing the scrotum with sharp pointed forceps to access the vas tubes. Both ends of the tubes are then cut, tied or cauterised to prevent the movement of sperm. Sperm production continues once the vas deferens sealed, and the sperm build up in these tubes can clog the system over a period of time.
The Metrocentre way of performing a vasectomy involves using fine instruments with two small access sites positioned precisely to access each testicle individually. A longer, reconstructive procedure is performed where the focus is on preserving the plumbing of the vas deferens to avoid the complication of haemorrhage and post vasectomy congestion pain; as well as to make it the most reversible if circumstances should ever change.
Traditional Vasectomy
A traditional vasectomy takes around 10 minutes to perform.
This technique uses either a scalpel or sharp forceps to access the vas tubes. It is usual to have either one central or two large incisions, the vas tube is cut and sealed (either burnt, tied or stapled) and sections of the vas deferens may be removed.
If large sections are removed and sutures or staples damage the blood supply in the scrotum, then a vasectomy reversal may be more difficult after this technique is used. By tying the ends attached to the testicles, blow outs and scarring of the fine storage tubules called the epididymis is more likely to cause chronic scrotal pain of varying severity (post vasectomy pain syndrome) and a more complex vasectomy reversal.
In one case we repaired, 10 metal staples (counted on ultrasound) were used in the vasectomy. This can cause significant collateral damage to important blood vessels, nerves and lymphatics that can increase the long-term risk of complications and lessen the chance of successful vasectomy reversal if there was a change of circumstance.
How does a vasectomy work - the Metrocentre Way?
Download our vasectomy guide to learn more about what to expect before, during and after your procedure.
Metrocentre Vasectomy Guide
How to get started with a vasectomy
At Metrocentre we strive to educate our patients about the various vasectomy procedures available in Australia, allowing you to make an educated decision on the treatment path you would like to pursue. Whether you’re just starting to explore vasectomy options or you’re ready to move forward, we’re here to support you every step of the way.
We have a number of pathways available, please see them below:
Same day Consult and procedure
Benefits of a Vasectomy the Metrocentre Way:
Reduction in Post Vasectomy Pain.
Preserves lymphatics, nerves, veins and arteries.
Retain normal function of the male reproductive organs.
Ready for a chat?
Call our friendly team on 1800 367 636 to book a consultation or book online.
Frequently Asked Questions
At Metrocentre we have created a gallery of some of the most commonly asked questions in relation to Vasectomies and the procedures we offer.
Our doctors are more than happy to answer any of your questions or concerns during your consultation – Book Now.
A true open-ended vasectomy should take at least 25 minutes to perform.
This procedure involves two tiny incisions to access the vas tubes. The tubes are then cut, and the testicular end is left opened and unsealed, with both ends of the tubes separated by layers of tissue within the scrotal sac by fine suturing. Sperm continues to be produced after the vasectomy so this fluid travels from the testicle up the vas deferens where it then flows out of the vas and into the tissues. The body reabsorbs this naturally. The testicular vas and the vas that leads to the prostate is reconstructed in a separate compartment to minimise the risk of failure.
As a result of this technique:
- A Reduced incidence of Post Vasectomy Pain (congestion) Syndrome, sperm do not suddenly build up in the testicle so the development of an inflammatory cascade, blow out and scarring of the fine epididymal tubules is avoided.
- Sperm flow is directed and absorbed under the skin rather than left to clog up the tubules.
- An open-ended vasectomised patient is unlikely to be aware that they have had a vasectomy unlike the closed ended vasectomy patients that often experience some form of aching and tenderness.
- Maximise potential of a successful future reversal if circumstances change.
- The nature of this technique prevents the build-up of sperm and the associated congestion (post vasectomy pain syndrome), a lower rate of postoperative pain, and a better potential for a vasectomy reversal in the future.
- Maintain normal function of the male reproductive organs.
- Maximise success of sterility by using a carefully considered reconstructive procedure.
- Preserve lymphatics, nerves and veins.
After your vasectomy surgery, you will be numb in that area for approximately 1-2 hours due to the local anaesthetic. We recommend applying cold packs to the area and rest for the remainder of the day. You may prefer to wear tighter underwear for support.
Over the next few days, you may have minimal or no swelling or pain. Panadol or Panadeine work well here. Keep away from anti-inflammatories – e.g. Nurofen for four (4) days after the procedure. We recommend taking at least 2 days off work to ensure a smooth recovery unless you have a desk job. After this time, you may return to work, however, you must avoid heavy lifting and strenuous activity for a week post-surgery. You will be able to resume sexual activity as soon as you feel comfortable to do so – usually around a week after surgery.
A vasectomy is partly covered by Medicare and the Medicare safety net may reimburse up to 85% of the procedure cost. The estimated Medicare rebate is $245.
It is important to note that sperm storage is not covered by Medicare, and this factor should be taken into consideration before undertaking this surgical procedure.
For patients who are technically difficult (experienced previous surgery or injury) or who want to be completely unaware of the procedure, twilight sedation is available in our purpose-built hospital in Miami, Gold Coast, offering private health rebates.
At Metrocentre, we use local anaesthetic. This means that most men can drive to and from the procedure. Many of our patients report that they experience little to no discomfort during and after the procedure.
If I am nervous or experience anxiety, can I receive additional anaesthesia?
In conjunction with local anaesthetic, we can additionally offer inhaled relaxant medication for men who are nervous about the procedure or more sensitive to pain. This can help you relax and feel more comfortable during the procedure. It is important to note that recovery time takes a little longer if this medication is used and you will not be able to drive for the rest of the day.
For patients who are technically difficult (experience previous surgery or injury) or who want to be completely unaware of the procedure, twilight sedation is available in our purpose-built hospital in Miami, Gold Coast, offering private health rebates.
If you are considering undertaking a vasectomy, at Metrocentre our highly experienced team are more than happy to consult with you directly, without a referral.
We can even conduct our consultations & procedures within the same day! We will send you all the information prior to your appointment, so you can understand all the information at hand. A separate consultation is recommended for those who have not had children, are not sure about the procedure or have significant past medical or surgical histories that are relevant to the scrotum.
At Metrocentre we have performed many successful vasectomy reversal procedures.
Although we do still view a vasectomy as a permanent procedure, there are higher success rates for a reversal with an open-ended vasectomy.
You may also wish to organise the storage of sperm before having your vasectomy procedure. At Metrocentre we are happy to help you organise this. Please advise our team in advance.

Our Team
Dr Chris Lekich leads our doctor team who provide the most effective and most reversible vasectomies with a highly specialised and very precise microsurgery technique.
It is important to learn about the different doctors and techniques available so you can make an informed choice about the type of vasectomy you wish to have, and the doctor you want to perform it.
Contact us
Get in Touch
"*" indicates required fields