Thinking about a vasectomy reversal? Here's what you should know first
Life circumstances can change, and so can your plans for the future. For men who have previously had a vasectomy and are now considering fathering children again or addressing post-vasectomy discomfort, vasectomy reversal may be an option worth exploring.
At Metrocentre, vasectomy reversals are performed using microsurgical techniques and refined surgical methods developed through the teachings of Professor Earl Owen. Our doctors perform reversals using the Owen 3-Layer Microsurgical Vasectomy Reversal Technique, a precise approach to reconnecting the vas deferens.
These procedures are performed in a dedicated microsurgical theatre at Miami Private Hospital on the Gold Coast.
What Is A vasectomy Reversal?
A vasectomy reversal is a microsurgical procedure designed to restore the flow of sperm into the semen after a vasectomy.
During the procedure, the vas deferens tubes that were previously interrupted during a vasectomy are carefully reconnected. This allows sperm produced in the testicles to once again travel through the reproductive tract and mix with semen.
Why Men Consider a Vasectomy Reversal
Men may explore vasectomy reversal for a number of reasons, including:
- A desire to have children after a previous vasectomy
- Changes in personal or family circumstances
- Addressing symptoms related to post-vasectomy congestion pain
Microsurgical vasectomy reversal is one option that may restore fertility by reconnecting the vas deferens using highly precise surgical techniques.
The Owen 3-layer Microsurgical vasectomy reversal technique
At Metrocentre, reversals are performed using the Owen 3-Layer Closure Technique, a microsurgical method developed by Professor Earl Owen.
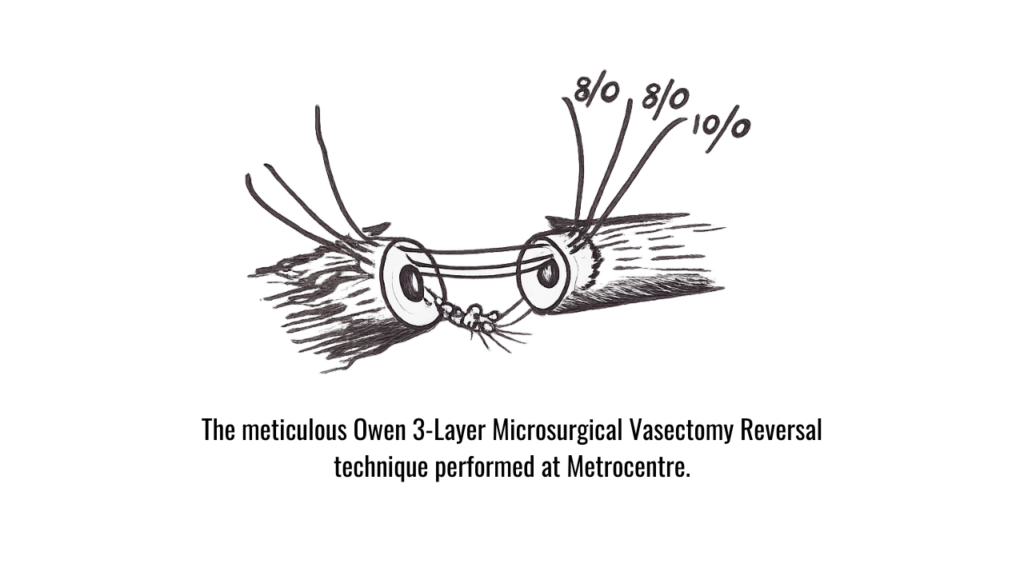
How the Owen 3-Layer Technique Works
This technique involves reconnecting the vas deferens using three precise layers of sutures:
- The inner lining (intima or mucosa)
- The middle muscular layer
- The outer supporting layer (adventitia)
These layers are carefully aligned and sutured under an operating microscope using extremely fine sutures.
Why Microsurgical Precision Matters
The vas deferens has an extremely small internal channel (approximately the width of two human hairs) which must be carefully aligned to allow sperm to pass through again.
Microsurgical techniques allows our doctors to perform this delicate reconstruction using high magnification and specialised instruments, helping ensure accurate alignment of the vas tubes.
Why Professor Owen's Techniques Still Matter
Professor Earl Owen pioneered many of the microsurgical principles used in modern vasectomy reversal procedures.
His work continues to influence how reversals are performed today, particularly through the Owen 3-Layer Technique, which focuses on precise tissue alignment and careful reconstruction.
The ongoing influence of the owen 3-Layer Technique
This approach has contributed to:
- Advances in microsurgical vasectomy reversal techniques
- Improved understanding of reproductive anatomy
- Training and mentorship of surgeons performing reversals today
Dr Chris Lekich trained extensively under Professor Owen, and this surgical mentorship continues to influence the techniques used at Metrocentre.
Vasectomy reversal at Metrocentre: what to expect
Vasectomy reversal is a highly precise procedure that requires specialised equipment and training.
At Metrocentre, reversals are performed at Miami Private Hospital, a purpose-built private hospital facility on the Gold Coast using an operating microscope and microsurgical instruments.
The Vasectomy Reversal Process
This process generally includes:


Is a vasectomy reversal right for you?
Every patient’s situation is unique, and several factors may influence whether reversal is an appropriate option.
Factors that may influence a reversal
These may include:
- The time since the original vasectomy
- The technique used during the vasectomy
- The condition of the vas deferens
- Overall reproductive health
At Metrocentre, vasectomies performed many years earlier, even decades ago may still be suitable for reversal depending on individual circumstances.
If you are considering reversal, a consultation can help determine whether this option may be appropriate for you.
Vasectomy Reversal vs IVF
For couples exploring fertility options after a vasectomy, both vasectomy reversal and IVF (in vitro fertilisation) may be considered. The most appropriate pathway depends on individual medical factors and should always be discussed with a qualified fertility specialist.
Differences Between Reversal and IVF
Vasectomy reversal is a microsurgical procedure that aims to reconnect the tubes (vas deferens) so sperm can again travel naturally. If successful, this may allow conception through intercourse over time.
IVF involves collecting eggs and sperm, fertilising them in a laboratory, and transferring an embryo into the uterus. This process bypasses the need for sperm to travel naturally.
The choice between these options is not one-size-fits-all. It depends on a range of factors including reproductive health, timing, and personal preferences.
Factors that may influence which option is appropriate can include:
- Age and fertility health of the female partner
- Previous fertility history
- Individual medical circumstances
Both options may be discussed during consultation when exploring fertility pathways.
Key Differences at a Glance
| Factor | Vasectomy Reversal | IVF |
|---|---|---|
| Approach | Restores natural sperm pathway | Assisted fertilisation in a lab |
| Conception method | Natural conception over time | Embryo transfer into uterus |
| Invasiveness | Surgical procedure for the male partner | Medical procedures for both partners |
| Time to pregnancy | Can vary and may take time | More controlled and time-specific |
| Female partner factors | Plays a significant role in success | Closely managed and assessed |
| Repeat attempts | Not typically repeated surgery | May involve multiple cycles |
| Suitability | May be suitable when conditions are favourable for natural conception | May be considered when other fertility factors are present |
Typical Recovery Guidance
In the early stages of recovery, the focus is on protecting the surgical area and supporting healing.
Patients are generally advised to:
- Rest and avoid strenuous physical activity, particularly in the first 1–2 weeks
- Avoid heavy lifting, exercise, or activities that place pressure on the groin
- Refrain from sexual activity for a period of time, as advised by your doctor
- Wear supportive underwear to help reduce discomfort and swelling
- Attend follow-up appointments to monitor healing and discuss recovery progress
Some swelling, bruising, or mild discomfort can occur after the procedure and typically improves over time.
Your doctor will provide specific post-operative instructions tailored to your situation. Following this guidance is important to support recovery and reduce the risk of complications.
If you have any concerns during your recovery, it’s important to contact your treating team for advice.
learn more about vasectomy reversal at metrocentre
A vasectomy reversal is a personal decision that requires careful consideration and access to clear information.
At Metrocentre, our focus is on precision microsurgery, careful tissue handling, and patient education throughout the process.
If you have previously had a vasectomy and are considering your options, our team can guide you through the consultation process.
Learn more about vasectomy reversal, watch our surgical information videos, or book a consultation with the Metrocentre team on the Gold Coast or in Brisbane.